By Simone J. van der Linden, MANP, BEd, RN; Leni van Doorn, MSc, MANP, RN; Judith P. van Eck, MANP, RN; Wanda Geilvoet, MANP, RN; and Greta Mulders, MANP, RN
A group of Dutch advanced practice nurses (APNs) describe their process of forming a peer review group (PRG) to share cases and provide feedback to one another. The purpose of the PRG is to help APNs expand their knowledge base and hone their clinical skills, with the ultimate goal of improving patient care.
In 1996, Dr. Els Borst, former Minister of Health of the Netherlands, proposed that specially trained master’s-prepared nurses assume certain tasks of physicians in order to help meet the growing need for healthcare in the midst of a physician shortage. In light of the increased number of elderly and chronically ill patients today, this need is even more pressing.1 The consequence of Dr. Borst’s proposal was the inauguration of the first Master’s in Advanced Nursing Practice (MANP) program in Groningen, the Netherlands, at the Hanze University of Applied Sciences in 1997.
Since that time, the training and the work accountability of advanced practice nurses (APNs) in the Netherlands have been extended. A major change occurred in March 2009, when Dutch APNs were granted official registration numbers and legal title protection. Nurses can be registered as APNs only after earning a master’s degree from a certified university and undergoing training on the job at a certified healthcare institute with a certified medical and nursing trainer.
Dutch APNs can be registered in one of five nursing specialties: (1) acute care in somatic disorders, (2) intensive care in somatic disorders, (3) chronic care in somatic disorders, (4) preventive care in somatic disorders and (5) mental health. Like physicians, APNs must attend conferences offering staff development workshops and be actively employed for at least 24 hours a week. In 2014, more than 2,500 APNs were registered in the Netherlands.2
After initial registration, APNs must re-register every 5 years to maintain an active license. Since 2010, one of the requisites for re-registration has been participation in peer review (PR). Guidelines of the Dutch Nursing Specialty Registration Board (DNSRB) require APNs to participate in a PR group (PRG) for at least 40 hours per 5-year period.3 In addition, to ensure competence and continuous professional development, periodic self-appraisal and peer feedback must be in place for all levels of nursing.4
Defining peer review
Peer review is a systematic process by which one assesses, monitors, and makes judgments about the quality of care provided to patients by others, as measured against established standards of practice.5,6 Nursing PR is an evaluation of one’s professional nursing practice, including identification of opportunities to improve care, by persons with the appropriate expertise to perform the evaluation.7 Because they undergo PR, APNs are a group of healthcare providers (HCPs) whose personal competencies in various nursing specialties are compared—with those of other APNs and with objective criteria—with the aim of improving daily practice.3 PR, recognized as a measure of accountability and a means to evaluate and improve practice,4 enhances development of the APN profession and improves the quality of patient care.
Peer review has multiple benefits for APNs. It facilitates an open and safe learning environment. It provides APNs with an opportunity to reflect on questions and problems together. Because of the interactive setting, APNs invariably learn something new.8 PR even offers APNs a break in an otherwise hectic workday. PR can help APNs evaluate the quality of care they have delivered, and gain insight into their greatest strengths and weaknesses as HCPs. With feedback and recommendations from the group, APNs can gain new knowledge and improve their skills.
Creating and working as a PRG
Because the APN profession is relatively new in the Netherlands, the nursing education department of the Erasmus Medical Center Rotterdam had no experience in starting or structuring a PRG. Five years ago, five pioneering APNs working on an internal medicine unit decided to create such a PRG. These APNs found several examples of PRGs in the literature and took the initiative in creating a framework, based on non-empirical research, that took into account the criteria requisites of the DNSRB.
To initiate an effective PRG, some basic steps are essential. The first step is to form a group of 3-5 APNs in the same specialty who have similar interests within their specialty. The next step is to elect a chair to serve a 1-year term. The chair then makes a yearly schedule so that members can plan to attend all PRG meetings. To meet the criterion of spending 40 hours in the PRG over 5 years, the group must meet for about 2 hours every 3 months.
At each meeting, members take turns serving as the contributor, who presents a case related to her work field. One week before the meeting, the contributor sends a recap of the case—along with corresponding literature, protocols, and guidelines—to PRG members so that they can read background material and analyze the case. Each case submitted for PR must have these elements:
- The patient’s presenting complaint, personal and family health history, and physical examination findings;
- An analysis of the case, with corresponding literature or guidelines to clarify or substantiate the diagnosis or the problem;
- A list of dilemmas that can occur or that did occur with the presented case, as well as learning points, and
- Learning objectives extracted from the presented case for discussion.
At the meeting, the contributor uses PowerPoint to present the case and then leads the discussion regarding dilemmas and learning goals. A member who is appointed secretary for each meeting takes notes and creates a report of the thoughts and views exchanged during the meeting. The report includes a summary of the case, the learning goals of the contributor, and feedback/recommendations from the group. After the meeting, the report is sent to the PRG members. Reports of PRG meetings are saved in a digital portfolio.
At the next PRG meeting, notes of the previous meeting are discussed. The chair asks the previous contributor whether she used feedback from the last PRG meeting and applied it to her practice. The process gives the contributor an opportunity to reflect on her own goals and improve the quality of her work.
Choosing the best method to present a case
Within the first year of the PRG’s existence, all five members had submitted a case. The group then met to determine the best format for presenting a case. The PRG considered three options: the testing method, the Balint method, and the research method. These methods were evaluated in terms of whether they enhanced the professionalism of the APN through the sharing of knowledge, expertise, and thoughts. The group was most satisfied with the testing method, which is particularly suitable for case study discussion and for evaluation of clinical guidelines and protocols. With this method, the group works together, sharing ideas and coming to an agreement on how practice can be improved. One downside of the testing method is that the personal learning goals of the APN are not included.
Gaining competencies
In the Netherlands, the focus of learning is to gain competencies. A framework used for the competency-based approach is that of the Canadian Medical Education Directives for Specialists (CanMEDS) (Figure).9 The CanMEDS framework describes seven different roles of an HCP: professional, communicator, collaborator, manager, health advocate, scholar, and, in the center, medical expert. APNs who have gained the first six competencies can become medical experts (the center of the honeycomb), but they cannot become medical experts if they fail to gain one of the six competencies surrounding the central competency. APNs need to enhance themselves in all seven competencies in order to become better HCPs.
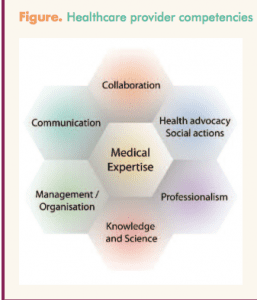
Achieving the best practice
A combined framework using both the testing method and the CanMEDS framework was determined to be the best practice. This combined framework was deemed to be the best way to prepare a case for discussion and to give the PRG and the contributor the clearest insight into the questions and learning issues provided by the case. The testing method is an ideal way to discuss problems or questions regarding certain procedures and guidelines within the safe confines of a group. In addition, each group member can impart information and share expertise via the group discussions, which can then be absorbed by the other members and translated into their own practices.
Discussion
The PRG found that, over a 4-year period, a combined approach—the testing method and the CanMEDS framework—constituted the best practice for structuring a case for discussion and determining the contributor’s own learning issues. The DNSRB also recommends use of CanMEDS competencies in this regard. If the combined framework does not work well for a given PRG, it may be related to poor group dynamics, lack of a safe environment, or a tendency for members discussing a case to highlight their feelings rather than their own practice. Some PRG members indicated that they sometimes felt vulnerable. It takes courage to learn from colleagues. According to Karas-Irwin and Hoffmann,4 a caring environment imbued with genuine respect enhances PRG interactions. By participating in a PRG, APNs in the Netherlands not only meet the needs and criteria of the DNSRB, but also enhance their professional skills and build their knowledge base.
Implications for APNs in the United States
Although there is no specific requirement to participate in PR as part of APN licensure in the United States, PR is recognized as an important component of practice and professional responsibility.10,11 The opportunity to come together as a small group of APNs with similar clinical practices and interests on a regular basis to review challenging cases provides a collegial environment for learning from each other. Peer assessments can play an important role in enhancing quality of care for complex patients with multiple interrelated chronic conditions, especially as seen in the U.S. with its aging population and the increasing prevalence of obesity and its co-morbidities.
Simone J. van der Linden is an APN in the Department of Hematology, Cancer Institute; Leni van Doorn is an APN in the Department of Medical Oncology, Cancer Institute; Judith P. van Eck is an APN in the Department of Medicine, Section of Endocrinology; Wanda Geilvoet is an APN in the Department of Medicine, Section of Endocrinology; and Greta Mulders is an APN in the Department of Hematology, all at Erasmus Medical Centre, Rotterdam, The Netherlands. The authors state that they do not have a financial interest in or other relationship with any commercial product named in this article.
Acknowledgment
The authors thank L. Maas, RN, MS, Rotterdam University, Master’s in Advanced Nursing Practice Program, Rotterdam, the Netherlands.
References
1. Statistics Netherlands. Dutch population expected to reach 17.5 million in 2038. cbs.nl/en-GB/menu/themas/
bevolking/publicaties/artikelen/archief/2008/2008-085-pb.htm
2. Dutch Nursing Association. 2013. venvnvs.nl/files/2014/09/Jaarverslag-VVN-VS-okt13-okt14-def.pdf
3. Dutch Nursing Specialty Registration Board. Intercollegiale Toetsing Verpleegkundig Specialisten. 2010.
verpleegkundigspecialismen.nl/Portals/45/20100203%20Intercollegiale%20Toetsing%20Verpleegkundig%20
Specialisten%20_3.pdf
4. Karas-Irwin BS, Hoffmann RL. Facing the facts: in-person peer review. Nurs Manage. 2014;45(11):14-17.
5. Sherwood GD, Brown M, Fay V, Wardell D. Defining nurse practitioner scope of practice: expanding primary care services. Internet J Adv Nurs Pract. 1997;1(2). geide.org/uploads/6/4/8/8/6488798/definingscope.pdf
6. Smith MA, Atherly AJ, Kane RL, Pacala JT. Peer review of the quality of care. Reliability and sources of variability for outcome and process assessments. JAMA. 1997;278(19):1573-1578.
7. Spiva LA, Jarrell N, Baio P. The power of nursing peer review. J Nurs Adm. 2014;44(11):586-590.
8. de Haan E. Leren met Collega’s. Uitgeverij Van Gorcum; 2009.
9. Frank JR, Jabbour M, Fréchette D, et al. Report of the CanMEDS Phase IV Working Groups. Ottawa, Canada: The Royal College of Physicians and Surgeons of Canada; 2005.
10. National Organization of Nurse Practitioner Faculties. Nurse Practitioner Core Competencies. 2012. c.ymcdn.com/
sites/www.nonpf.org/resource/resmgr/competencies/npcorecompetenciesfinal2012.pdf
11. National Association of Nurse Practitioners in Women’s Health/Association of Women’s Health, Obstetric and Neonatal Nurses. Women’s Health Nurse Practitioner: Guidelines for Practice and Education, 7th Edition. Washington, DC: NPWH/AWHONN; 2014.
We invite readers to submit articles on Professional development topics—for example, processes that foster learning or quality improvement in clinical practice or that promote the business aspect of being an NP. Please see our Guidelines for Authors for more information about this short-form article option.


1 Comment. Leave new
An excellent, insightful article, thank you. It will guide other HCP who seek to form peer review groups that take nursing case review & reflection, competencies, policies & procedures to a more attuned practice level. Empowering nurses in constructive learning environments enhances engagement, the route to improving
patient safety & quality care.