Polycystic ovary syndrome (PCOS), a complex disorder affecting reproductive-aged females, presents challenges for equipping patients with knowledge and tools to manage their condition. The authors examined the feasibility of conducting a group visit program in a college health setting for women with PCOS, and ascertained whether these visits might effectuate favorable changes in these women’s self efficacy and health practices.
Polycystic ovary syndrome (PCOS), the most common endocrine disorder of reproductive-aged women,1 affects up to 18% of these women.2 This complex, chronic, multisystem syndrome is manifested by anovulation, irregular menses, hyperandrogenism, and infertility.2 In addition, it is associated with an increased incidence of obesity and other risk factors for cardiovascular disease.3
Primary treatment for PCOS entails following a healthful diet and a regular aerobic exercise regimen, alone or in combination with medications—including hormones.2,4 Because of the wide range of symptoms, many patients with PCOS seek care from multiple healthcare providers (HCPs), including primary care providers and specialists in gynecology, dermatology, and endocrinology.1,5 As a result, patients may receive inconsistent recommendations from the providers, leading to frustration and confusion.1 Brevity of the HCP visits may also preclude patients from receiving clear instructions regarding PCOS management or clarification of any inconsistencies in the HCPs’ recommendations.
Use of a group visit model, in which several patients meet simultaneously with an HCP and hold discussions, can improve patients’ self-management behaviors. According to Bandura’s social cognitive theory, a person’s health behaviors are influenced by knowledge of health risks, belief in one’s own ability to make changes (self-efficacy), belief that one’s efforts will make a difference (outcome expectancy), self-determined health goals, and perceived facilitators and impediments to health behaviors.6 In the group visit, each of these factors can be addressed, giving patients the opportunity to increase their knowledge, solidify their expectations for specific outcomes of their behavioral efforts, interact with others with similar challenges, and aim to meet their personal health goals.
The group visit model has been implemented in caring for patients with chronic diseases since 1997, with high levels of success, particularly in improving self-management.7,8 Use of group visits has been shown to lead to satisfaction, improved self-efficacy and knowledge, and beneficial lifestyle modifications in patients with chronic conditions9,10 such as diabetes,11-16 heart failure,17 hypertension,18 metabolic syndrome,19 and childhood obesity.20 In addition, researchers have found evidence of improved quality of life and decreased loneliness and depression with use of group visits.21 Given these successes, use of the group visit model might improve the care of patients with PCOS.1 To date, no studies examining the use of this model in patients with PCOS have been published.
Like other patients with chronic conditions, patients with PCOS can likely benefit from being actively involved in the day-to-day management of their condition. To do so, they need to acquire the skills needed to perform self-management behaviors. Modeling and social persuasion, which can occur through group visits, are powerful means for developing these skills and improving self-efficacy.22 As peers discuss their own efforts and problem-solving behaviors, they can enhance each other’s skills in solving problems, making decisions, utilizing resources, building partnerships with HCPs, and taking action.22 As skills increase, their self-management should improve and likely translate into better health outcomes.
Purpose
The purpose of this pilot study was to evaluate the use of group visits in patients with PCOS. Primary aims were (1) to assess the feasibility of implementing group visits in a university setting, (2) to evaluate changes in patient confidence in their ability to self-manage PCOS (self-efficacy), and (3) to ascertain whether participants begin to engage in health-promoting diet and exercise behaviors.
Methods
Approval was obtained from the Institutional Review Board and from the university health clinic where the project was conducted. Participants were recruited by secure messaging through the electronic patient portal or by personal communication at office visits. Patients were invited to participate if they were non-pregnant, post-menarchal, premenopausal females aged 18 years or older with a diagnosis of PCOS; seen in the student health clinic within the past academic year; and actively enrolled at the university. Participants, who could be of any race or ethnicity, were required to speak and read English. Forty-three patients met inclusion criteria. These patients and three others identified by clinic providers during recruitment were invited to participate. A total of nine patients accepted the invitation.
Group visit basics
Patient visit fees were waived for the three group visits, which were held in a conference room at the clinic. Visits were held monthly on two different weekday afternoons for three consecutive months. Participants were invited to attend whichever weekday group was most convenient for them. Each visit lasted 90-120 minutes and included measurement of vital signs; group interaction, education, and goal setting; and focused individual consultations. The primary investigator (PI), who was a nurse practitioner (NP), also served as the HCP, prescriber, and group leader. As an incentive, participants were entered into raffles for additional services (e.g., a visit with a dietitian) and for one of two $25 Amazon gift cards following the final online survey.
Visit 1
At the first visit, held in October 2015, participants completed written informed consent and signed authorization to allow use of personal health information for the study. Then they completed a written pre-intervention survey consisting of relevant items from the Chronic Disease Self-Efficacy Scale,23 answered reproductive and menstrual history questions to assess menstrual cycle characteristics,24 and answered diet and exercise behavior questions adapted from the National Health and Nutrition Examination Survey (NHANES) 2007-2008 Questionnaire.25 The pre-intervention survey included questions about demographics and interest level in specific aspects of PCOS. While participants were completing the survey, each person was pulled aside for measurement of height, weight, blood pressure, and heart rate, and was asked to state the first day of her last menstrual period.
The PI welcomed the participants and discussed the study purpose. The participants introduced themselves. The PI presented an overview of PCOS and associated risks, including the most common symptoms and basic management strategies, and provided a list of community resources for women with PCOS. A group discussion on personal experiences with PCOS, symptom management, and individual goal setting was held. A brief explanation of SMARTER (specific, measureable, achievable, relevant, time-bound, engaging, rewarding) goal setting was provided.26 Each group member chose one health behavior goal for the month related to the visit discussion, and rated her confidence in her ability to complete it on a scale of 0 10. For participants who rated their confidence <7, the group discussed barriers and strategies to overcome them. Brief one-on-one consultations were held, including ordering of prescriptions, laboratory tests, and/or referrals needed.
Visit 2
The second visit occurred 1 month later in the same conference room. Two newly identified patients with PCOS were invited to participate, bringing the total number of participants to 11. The new patients completed written consent and pre-intervention surveys and were given paper copies of the information provided at the first visit. Vital signs were measured in all participants. The group discussed suggestions for overcoming barriers to goal attainment. A registered dietician led a 20-minute educational discussion about diet and exercise strategies for weight loss. The PI briefly discussed other PCOS-associated risks, including sleep apnea and dyslipidemia, and group members joined in. Each participant set new goals for the month related to diet or exercise and discussed potential barriers to overcome. Brief individual meetings with the PI were held as needed.
Visit 3
The third visit was held 1 month later. Vital signs were measured. A follow-up discussion of participants’ experiences with their goals was held. A 20-minute educational discussion about depression and coping with chronic disease was conducted. The discussion in the Wednesday session was led by the PI and in the Thursday session by a psychiatric and mental health NP. The PI briefly presented new trends in PCOS management. Goal setting and group discussion followed. Brief one-on-one visits with the PI were held to ensure a plan for follow-up. While these visits were being conducted, participants completed post-intervention surveys. This survey posed the same questions as the first survey to gauge self-efficacy and health behavior practices, and asked participants to rate their experiences with the group visits. Self-efficacy scores were based on Likert scale questions with 0 representing not confident at all and 10 representing totally confident.
Three months after the final visit, a brief version of same post-intervention survey was sent electronically via Qualtrics to participants. A raffle for two $25 Amazon gift cards was available to survey completers.
Data analysis
Pre- and post-intervention data were entered into Microsoft Excel and then transferred to IBM SPSS Statistics Version 24 for analysis. Descriptive statistics were analyzed to report group demographics and to compare pre-intervention data with immediate post-intervention data and 3-month post-intervention data. Effect sizes were calculated using Cohen’s d, with small effect defined as 0.2, moderate effect as 0.5, and large effect as 0.8. Effect size was used rather than inferential statistics because it is not as affected by sample size as are tests of significance, and it better represents how much change occurred rather than simply whether or not change occurred.27
Results
The groups consisted of 11 participants, who could attend either weekday session. Group 1 attendance ranged from 3 to 5 participants, and Group 2 attendance ranged from 4 to 7 participants. Nine participants completed post-intervention surveys at visit 3 and were included in pre- and post-intervention comparative analysis. Seven participants completed the final survey 3 months later. Some participants who completed the final survey did not complete the visit 3 survey. In terms of overall adherence, 64% attended all 3 sessions, 18% attended 2 sessions, and 18% attended 1 session.
Participants ranged in age from 20 to 32 years (mean, 24.09±3.986 years) and reported experiencing PCOS symptoms for a mean of 6.82 years. Eight (72.7%) identified their race as white and 3 (36.4%) as other. Three identified their ethnicity as Hispanic (27.3%). Mean body mass index (BMI) at baseline was 30.85 (range, 19-52). All but one participant were nulliparous. Reported symptoms of PCOS were weight gain (64%), irregular periods (73%), acne (82%), excessive hair growth
(100%), hair loss (45%), and depression (27%). Participants expressed interest in these topics (n, %): irregular periods (8, 73%), hirsutism (11, 100%), acne (10, 91%), weight management (11, 100%), fertility (10, 91%), coping with a chronic condition (11, 100%), depression (10, 91%), and risk for developing other diseases (11, 100%). Other topics of interest were “dealing with healthcare and issues with obtaining hormones” (1, 9%), “causes” (1, 9%), and “diet” (1, 9%).
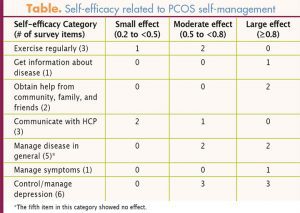
The magnitude of effect of the visits on self-efficacy items ranged from large to small. Effect size using Cohen’s d showed a large effect size in 9 items (43%), a moderate effect size in 8 items (38%), and a small effect size in 3 items (14%) (Table). The 3-month post-intervention follow-up survey showed that these effects decreased overall but were still evident on several items. Over the course of the intervention, actual health practices did not change.
In rating their experience with the visits, all participants rated their expectations as “met” (n = 4, 44%) or “exceeded” (n = 5, 56%). In terms of new knowledge attainment, all participants rated their learning as either “quite a bit” (n = 5, 56%) or “a great deal” (n = 4, 44%). Comments were positive, with several participants extolling the usefulness of the diet information. Others welcomed information on the hormonal effects of PCOS, the impact of PCOS on future fertility, depression, and coping. Two participants said the most useful thing was meeting together in a group. Suggestions for improvement included continuing the groups for at least a year, having larger groups, providing blood testing, and allowing more opportunity for participants to bond with each other.
Discussion
This pilot study aimed to evaluate the use of a group visit model to improve self-management of PCOS. Researchers found that the group format was feasible in the college health setting and that participants’ responses were quite positive. Participants enjoyed the sessions and learned new information.
A comparison of pre- and immediately post-intervention self-efficacy using the Chronic Disease Self-Efficacy Scale showed positive effects in most areas. Categories of self-efficacy showing large positive effects included getting information about the disease; obtaining help from community, family, or friends; communicating with one’s HCP; managing one’s health condition in general; managing symptoms; and controlling or managing depression. Small to moderate positive effects were seen on some items within each of these aforementioned categories, as well as in self-efficacy to exercise regularly. Overall, baseline scores were fairly high, allowing little room for improvement in some aspects of self-efficacy. In addition, all of the participants were already established patients of the student health clinic, had received some PCOS education, and had a relationship with their HCP before beginning the group sessions. Given the large effect sizes observed in some variables, one may conclude that group visits have the potential to improve self-efficacy in patients with PCOS.
However, the improvement in self-efficacy did not translate into changes in health behaviors. Despite the group visits, participants did not make greater attempts to lose weight, engage in moderate or vigorous exercise, or follow a recommended diet.
Participants’ comments and group experience ratings were highly positive. Although behavior change did not occur during the short time frame of the intervention, the participants found it to be a favorable experience. Perhaps learning itself may serve as a step toward making behavior changes later on, which might ultimately bring about an improvement in their BMI. In addition, participants acquired new information and were satisfied with the group experience.
Limitations
Limitations of this pilot study included the small sample size and lack of control group, which affected the ability to find significant changes in outcomes; the short follow-up, which limited the ability to establish meaningful behavior change; and possible survey fatigue. With regard to evaluating the results, the small number of participants precluded the determination of statistical significance; therefore, as mentioned earlier, effect size was used instead. However, because the participants reporting on surveys 1, 2, and 3 differed, it is not known whether the calculated effect sizes over- or underestimated the noted effects. These effects followed the pattern expected in that they were greatest immediately following the intervention and decreased over time after the group visits ended. In addition, some participants who completed the final online follow-up survey had not attended all the sessions or completed the visit 3 survey, so their improvement in self-efficacy was expected to have been lower than that experienced by participants who attended more sessions and completed the survey at the conclusion of visit 3. This was reflected in the decreased effect sizes at 3 months following the intervention.
The short follow-up may have affected the ability to observe change, particularly in behavioral outcomes. Behavioral changes are difficult to implement and require extended time to become habitual. Initiation and maintenance of lifestyle changes are most effective with long-term and frequent contact with patients,28 which was outside the scope of this study. Despite these limitations, some large effects were noted, suggesting the potential of this intervention.
Conclusion
Usual care for patients with PCOS (i.e., individual office visits) can be rushed, complex, and confusing. Many patients seek care from multiple HCPs and can receive conflicting messages. Patients with PCOS need to engage in daily diet and exercise behaviors that support their health. Findings of this study support those of previous studies showing that group visits can improve self-efficacy in managing chronic conditions. The group setting provides modeling of health behaviors, education, and skill building necessary for self-management. This pilot study has established a basis for larger future studies and supports the feasibility of group visits for PCOS care in the college health setting.
Elizabeth Harrison is Assistant Clinical Professor at Texas A&M Health Science Center in Bryan, Texas. Helen W. Lach is Professor at Saint Louis University in St. Louis, Missouri. The authors state that they do not have a financial interest in or other relationship with any commercial product named in this article.
References
- Moore A, Caldwell J. The importance of collaboration in treating chronic disease: a focus on PCOS and group medical visits. Womens Health Care. 2011;10(9):10-18.
- Moran LJ, Hutchison, SK, Norman RJ, Teede HJ. Lifestyle changes in women with polycystic ovary syndrome. Cochrane Database Syst Rev. 2011;7:1-43.
- Kahal H, Atkin SL, Sathyapalan T. Pharmacological treatment of obesity in patients with polycystic ovary syndrome. J Obes. 2011; 2011:402052.
- Legro RS, Arslanian SA, Ehrmann EA, et al. Diagnosis and treatment of polycystic ovary syndrome: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2013;98(12):4565-4592.
- Colwell K, Lujan ME, Lawson KL, et al. Women’s perceptions of polycystic ovary syndrome following participation in a clinical research study: implications for knowledge, feelings, and daily health practices. J Obstet Gynaecol Can. 2010;32(5):453-459.
- Bandura A. Health promotion by social cognitive means. Health Educ Behav. 2004;31(2):143-164.
- Beck A, Scott J, Williams P, et al. A randomized trial of group outpatient visits for chronically ill older HMO members: the Cooperative Health Care Clinic. J Am Geriatr Soc. 1997;45(5):543-549.
- Scott JC, Conner DA, Venohr I, et al. Effectiveness of a group outpatient visit model for chronically ill older health maintenance organization members: a 2-year randomized trial of the cooperative health care clinic. J Am Geriatr Soc. 2004;52(9):1463-1470.
- Quality Enhancement Research Initiative. Evidence-based Synthesis Program. Shared Medical Appointments for Chronic Medical Conditions: A Systematic Review. Washington, DC: Department of Veterans Affairs (US); 2012.
- Murray JL, Everson K. Group medical visits and lifestyle modifi cation. J Fam Pract. 2005;54(1):64.
- Dobbins VM. Evaluation of Group Medical Visits in Improvement of Diabetes Self-Management. West Virginia University; 2012. E-book available from: CINAHL Plus with Full Text, Ipswich, MA.
- Esden JL, Nichols MR. Patient-centered group diabetes care: a practice innovation. Nurse Pract. 2013;38(4):42-48.
- Housden L, Wong ST, Dawes M. Effectiveness of group medical visits for improving diabetes care: a systematic review and meta-analysis. CMAJ. 2013;185(13):E635-E644.
- Liu S, Bi A, Fu D, et al. Effectiveness of using group visit model to support diabetes patient self-management in rural communities of Shanghai: a randomized controlled trial. BMC Public Health. 2012;12:1043-1053.
- Taveira TH, Friedmann PD, Cohen LB, et al. Pharmacist-led group medical appointment model in type 2 diabetes. Diabetes Educ. 2010;36(1):109-117.
- Trento M, Passera P, Borgo E, et al. A 5-year randomized controlled study of learning, problem solving ability, and quality of life modifications in people with type 2 diabetes managed by group care. Diabetes Care. 2004;27(3):670-675.
- Yehle KS, Sands LP, Rhynders PA, Newton GD. The effect of shared medical visits on knowledge and self-care in patients with heart failure: a pilot study. Heart Lung. 2009;38(1):25-33.
- Edelman D, Fredrickson SK, Melnyk SD, et al. Medical clinics versus usual care for patients with both diabetes and hypertension: a randomized trial. Ann Intern Med. 2010;152(11):689-696.
- Greer DM, Hill DC. Implementing an evidence-based metabolic syndrome prevention and treatment program utilizing group visits. J Am Acad Nurse Pract. 2011;23(2):76-83.
- Gimpel N, Teng R, Billmeier T, et al. Evaluating the impact of the Fitness in Nutrition and Exercise (FINE) Program within Shared Medical Appointments (SMA) on reducing childhood obesity in a community-based clinic. Texas Public Health J. 2010;62(2):28-31.
- Geller JS, Orkaby A, Cleghorn GD. Impact of a group medical visit program on Latino health-related quality of life. Explore (NY). 2011;7(2):94-99.
- Jeon SM, Benavente V. Health coaching in nurse practitioner-led group visits for chronic care. J Nurse Pract. 2016;12(4):258-264.
- Lorig K, Stewart A, Ritter P, et al. Outcome Measures for Health Education and Other Health Care Interventions. Thousand Oaks, CA: Sage Publications; 1996.
- Wei S, Schmidt MD, Dwyer T, et al. Obesity and menstrual irregularity: associations with SHBG, testosterone, and insulin. Obesity (Silver Spring). 2009;17(5):1070-1076.
- CDC. National Center for Health Statistics. NHANES 2007-2008 Questionnaire Data.
- MacLeod L. Making SMART goals smarter. Physician Exec. 2012;38(2):68-70, 72.
- Coe R. It’s the Effect Size, Stupid: what effect size is and why it is important. Presented at: Annual Conference of the British Educational Research Association; 12-14 September 2002; University of Exeter, England.
- Wing RR, Goldstein MG, Acton KJ, et al. Lifestyle changes related to obesity, eating behavior, and physical activity. Diabetes Care. 2001;24(1):117-123.

